Abstract
Background:
What is Laparoscopically Assisted Spinal Surgery: One of the newest frontiers of videolaparoscopic surgery is spinal surgery, which necessitates the collaboration of both the spinal surgeon and the laparoscopic general surgeon. Let’s know more about What is Laparoscopically Assisted Spinal Surgery.

Data Base:
We present our findings from 76 laparoscopic spinal surgery cases performed utilising both a transperitoneal and a retroperitoneal technique. The technical complexities and problems are thoroughly described. Let’s know more about What is Laparoscopically Assisted Spinal Surgery.
Conclusions:
A transperitoneal approach was used on 51 patients, with an average operating time of 117 minutes. The average length of stay for uncomplicated cases was 4.4 days. Five patients needed to be converted. Except for one, all of the patients had L5-S1 level surgery. A retroperitoneal technique was used on 25 patients, with a 150-minute operating time and a 5.7-day stay. A two-balloon approach was used to reduce conversions. Multiple level surgery with nearly infinite fusion devices is possible with the retroperitoneal technique. All of the advantages of minimally invasive surgery are available to the spinal surgeon with laparoscopically assisted spine surgery Let’s know more about What is Laparoscopically Assisted Spinal Surgery. .
INTRODUCTION
Despite the fact that general surgeons were among the last to adopt videoendoscopy, the advances made since the initial laparoscopic cholecystectomy have been nothing short of phenomenal. Furthermore, practically every general surgeon in the globe has been retrained as a result of this exponential development in general surgical applications.
Although progress appears to be slowing, a multidisciplinary approach allows surgeons of various disciplines to continue to broaden their perspectives. This attitude of collaboration is evident in the rapidly emerging specialty of laparoscopically assisted anterior spine surgery. In 1991, Obenchain published his sentinel case, demonstrating the theoretical benefits of laparoscopic lumbar discectomy in practise. 1 In 1995, animal and early clinical investigations were published. Let’s know more about What is Laparoscopically Assisted Spinal Surgery.
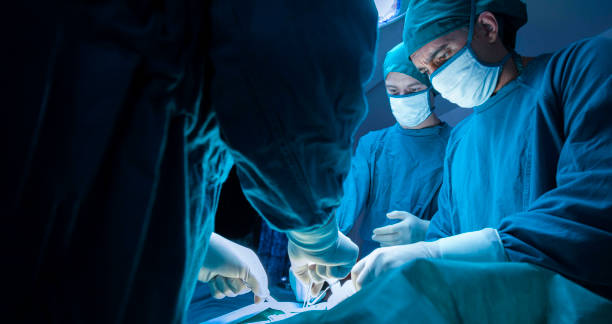
Despite the fact that many spine surgeons, orthopedists, and neurosurgeons have the technical abilities and training to expose the anterior spine, few have the laparoscopic experience to execute these treatments utilising minimally invasive methods. From single-level transperitoneal L5-S1 exposures to multiple-level thoracoabdominal approaches, we have a lot of expertise with open anterior spine methods. We have favoured fully extraperitoneal access over the past six years, using either a left flank or left paramedian incision.
The authors have had experience with laparoscopically aided anterior lumbar spine exposure during the previous two years, first utilising transperitoneal approaches with two distinct operating systems, and more recently with a completely extraperitoneal gasless approach. Experience and new technology, like with other early endoscopic operations, make these “techniques in evolution.” Let’s know more about What is Laparoscopically Assisted Spinal Surgery.
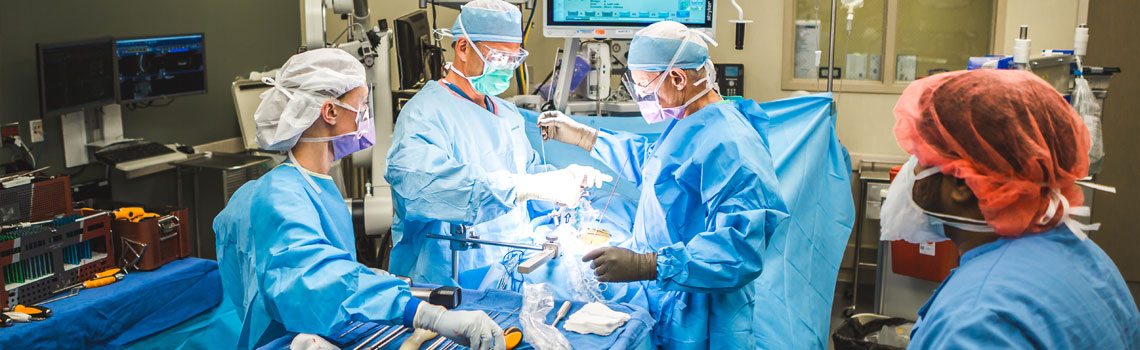
METHODS
Transperitoneal Approach:
The patient is positioned supine with arms crossed and fastened across the chest for continuous cross-table lateral fluoroscopy. When a steep Trendelenberg posture is necessary, shoulder bracing are employed to prevent slipping. Following the induction of general endotracheal anaesthetic, a Foley catheter is inserted. A 10 mm trocar and a 0 degree laparoscope are inserted at the umbilicus once pneumoperitoneum has been established. In the right hemi-abdomen, two 5 mm trocars are placed: one opposite the umbilicus and the other in the right lower quadrant. Let’s know more about What is Laparoscopically Assisted Spinal Surgery.

With the use of a steep Trendelenberg posture and laparoscopic Kittner dissectors, the small bowel is pushed out of the pelvis. With a laparoscopic Babcock clamp, the sigmoid colon is retracted superiorly and to the patient’s left by a 10 mm trocar inserted in the midline across the L5-S1 interspace. The sacral promontory’s peritoneum is dissected vertically, and the L5-S1 disc is identified. The disc space is cleared widely with gentle mobilisation of the common iliac veins, and all dissection is done vertically to avoid the hypogastric nerves. The middle sacral vessels are taken with bipolar cautery, and the disc space is cleared widely with gentle mobilisation of the common iliac veins. Let’s know more about What is Laparoscopically Assisted Spinal Surgery.
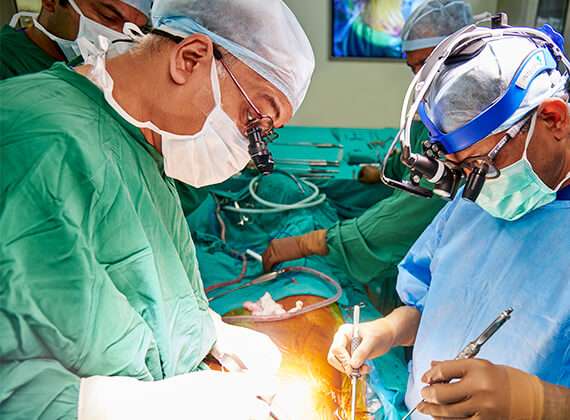
Fluoroscopy is used to confirm the centre of the targeted disc, and the entire spinal component of the treatment is done under X-ray control. The disc core is trephined and dilated, the “tubes” are docked onto the disc, the discectomy is performed, and bone dowels or cage devices are implanted and fastened. The trocars are removed after the spinal procedure, and the bigger fascial wounds are closed before the skin incisions. The patient is rotated and a posterior operation is conducted when required. Let’s know more about What is Laparoscopically Assisted Spinal Surgery.
Extraperitoneal:
The patient is repositioned in a supine position, arms crossed across the chest. The anterior rectus sheath is incised, the muscle is withdrawn, and the posterior rectus sheath is identified by a subumbilical incision. A kidney-shaped balloon dissector is positioned to the left of the midline and inflated, aiming towards the pubic symphysis. The retroperitoneal area is then accessed, either with finger dissection or an Optiview trocar, by a tiny incision immediately medial to the tip of the left 12th rib. Let’s know more about What is Laparoscopically Assisted Spinal Surgery.
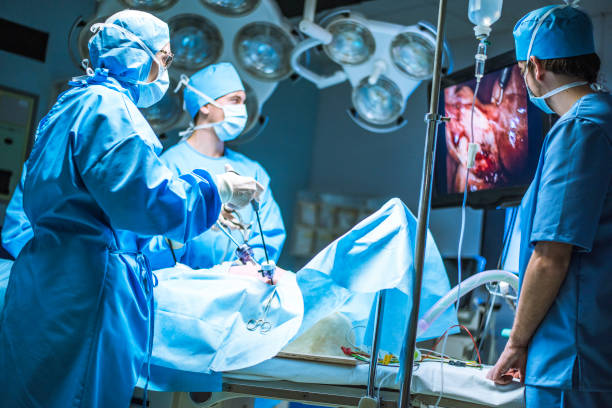
A second kidney-shaped balloon is inserted into the preperitoneal region and inflated, aiming for the pubis. This balloon is withdrawn and replaced with a balloon-tipped trocar, allowing for retroperitoneum insufflation. A 5 mm trocar is inserted just anterior to the anterior superior iliac spine to facilitate blunt dissection to join the two extraperitoneal areas produced by the balloons.
This incision is used if bone harvesting has been done. The lifting devices are then put in the 12th rib location, together with the laparoscope, utilising a gasless technique. The iliac crest site is extended to 10 mm, and the disc gaps are dissected using a gasless trocar and two Kittner dissectors. Fluoroscopy is utilised to confirm the operative location if necessary, however it is not required during a spinal procedure.
The operating incision for the spine surgeon is created in the lower midline, giving access to midline retractors and other surgical equipment. A typical discectomy and fusion can be performed utilising any open approach. Fascial incisions and skin are closed at the end of the treatment.
Read More:
| Sciatica Causes |
| Sciatica Surgery 2022 |
| What Is Cervicogenic Headache? |
| Acupuncture for Chronic Stiff Neck |
| All About Neck Pain |
| Anti-Inflammatory Foods to Try for Neck Pain |
| Spine Structure and Function |
RESULTS

Between August 1994 and December 1996, two spinal surgeons conducted 76 laparoscopically assisted anterior spinal discectomies and fusions. There were 51 transabdominal procedures and 25 retroperitoneal procedures in the previous 12 months.
There were 19 males and 32 women in the transperitoneal group, with an average age of 42 years (15-82). Only one patient had a L4-5, L5-S1 surgery completed. Fifty of the 51 surgeries were conducted in the L5-S1 disc region. The average weight of the participants was 173 pounds (78.6 Kg.). The Danek and Spinetech devices were used in all of the patients, and both relied on bone dowels for fusion. BAK devices (interbody fusion devices, SpineTech Co.) and cages were not utilised. The anterior approach took an average of 117 minutes (55-235) to complete.

Pseudoarthrosis was the reason for surgery in 44% of cases, followed by degenerative disc disease (36%), annular rupture (12%), and spondylolisthesis (8%). (Table 2). Half of the people in the front group had already had spinal surgery. Patients were rotated in roughly one-third of the instances, and a posterior surgery was conducted. The average length of stay for the total research group (3-17 days) was 5.3 days, but only 4.4 days (3-7) for those without difficulties.
There were five occurrences that necessitated the use of an open approach. A almost infantile pelvis in one exceedingly little lady was too small to admit laparoscopic equipment. Two conversions were due to adhesions, one due to thick adhesions from previous abdominal surgery and the other due to disc inflammation preventing safe iliac vein dissection. Two further conversions were caused by a low bifurcation of the great vessels and an injury to the right iliac vein.

There was one episode of pulmonary embolus, ileus, mechanical small intestinal blockage, and bone plug displacement in the hospital (Table 5). Three late problems necessitated re-operation. Bone plugs were displaced in two cases. The misplaced bone plug impinged on the left iliac vein, creating deep venous thrombosis, necessitating plug removal and venorraphy in one patient; in the other, the displaced bone plug impinged on the left iliac vein, causing deep venous thrombosis, necessitating plug removal and venorraphy (Table 6). A positive fungal culture in one patient necessitated an open anterior procedure on the third postoperative day. There were no deaths in this incident.
A balloon-assisted retroperitoneal approach was used in twenty-five patients. Three patients in this group had a multi-level operation, L4-5, L5-S1. Fourteen of the participants used a single balloon, while eleven used two balloons. The anterior phase of the surgery took an average of 150 minutes (120-180) in the 25 patients who received a retroperitoneal approach. A combination anterior-posterior surgery was performed on two-thirds of the patients. Initially, we simply utilised one balloon to produce the posterior and lateral spaces, while dissecting the peritoneum anteriorly using a blunt midline incision.

Because the peritoneum is violated and the small bowel enters the preperitoneal region, all exposure is lost once the peritoneum is violated and the small bowel enters the preperitoneal space, this anterior dissection was more challenging and was responsible for all of our conversions. Five (20%) of the patients required open surgery due to peritoneal tears that could not be repaired. These tears were discovered in the first single-balloon group; no tears or conversions were identified in the double-balloon group (Table 8).
5.7 days was the average length of stay (4-10). The only problems in this group were ileus and partial small bowel blockage. In one patient, a left iliac vein injury was treated, and the case was concluded without conversion. There were no long-term problems or fatalities .
DISCUSSION
In collaborative spinal surgery, the spine surgeon is solely responsible for patient selection and operation indications. The patient’s appropriateness for a significant intra-abdominal or major retroperitoneal surgery, as well as incision location, should be assessed, taking into account previous surgical and medical history. Long-term outcomes of spine surgery need at least two years of follow-up and are outside the realm of a general surgeon’s expertise.
The general surgeon’s role in laparoscopically assisted spine surgery is to ensure that the spine is exposed safely and efficiently (Table 10). An ideal approach would also allow a general surgeon to swiftly and securely expose numerous levels of the lumbar spine. Outcome endpoints are difficult to quantify in even the most comprehensive orthopaedic and neurosurgery evaluations.
The transperitoneal method arose first, much like the evolution of laparoscopic hernia, since it is the easiest to learn. Unfortunately, in the gas environment, the spine surgeon is confined to devices that rely on tubes to maintain pneumoperitoneum.
The discectomy is restricted by necessity, as are the options for achieving a stable fusion. Furthermore, only the L5-S1 interspace is accessible with anterior exposure. Although larger amounts of exposure are achievable, significant vascular problems become more common.
The retroperitoneal technique avoids all of the drawbacks of transperitoneal exposure while also making access to numerous levels of the spine considerably simpler. Furthermore, the gasless environment allows spine surgeons to employ all of their traditional equipment as well as time-tested fusion procedures while using modern gear.
Unfortunately, the peritoneum must be cleaned beyond the rectus muscle to beyond the midline when using the retroperitoneal technique. Small bowel can enter the retroperitoneal area through any hole in the peritoneum, making the surgery difficult. We quickly discovered that this was the most challenging dissection and that it was solely responsible for conversions to an open approach.
The anterior peritoneal dissection is finished quickly with the two-balloon approach, exactly as it is with the TEP (totally extraperitoneal) hernia procedure: we have had no conversions to open since its implementation. Furthermore, the gasless technique offers for more flexibility in dealing with difficulties during disc space dissection, which is usually diseased.
Bleeding from an iliac vein is usually straightforward to control, while pneumoperitoneum makes continuous suction and clip procedures hard.
Prospective randomized studies will be required once procedures for laparoscopically assisted spine surgery have been developed. Unfortunately, evaluating the results of spine surgery is challenging. Of fact, the success of a fusion is simply one of the outcomes.
Back pain relief and resumption of regular activities are the most difficult to quantify. Minimally invasive approaches, on the other hand, will allow anterior treatments to be conducted at numerous levels with reduced morbidity. These better outcomes will need a true collaborative effort between an experienced laparoscopic general surgeon and a spine surgeon who is ready to venture into the minimally invasive realm.

Laparoscopically Assisted Spinal Surgery At Gwalior
Dr Vipin the managing director of KLM Group. He is a well-known gold-medalist Orthopedic Surgeon In gwalior, strongly reputed for his trusted and focused attitude our rich knowledge and experience, be assured of quality healthcare and world-class medical services in Orthopaedic, Spine care In gwalior, Ophthalmology, X-ray & Diagnostics services along with physiotherapy services.
Book Your Consultation
Website: https://tinyurl.com/yyzvwmck
Email: info@klmgrou p.org
Ph: 0751-4000721,Mob: 7804826825
Address: 12, Saraswati Nagar, University Road, Near Silver Estate, Thatipur,

